-
 Specific Antimicrobial Activities Revealed by Comparative Evaluation of Selected Gemmotherapy Extracts
Specific Antimicrobial Activities Revealed by Comparative Evaluation of Selected Gemmotherapy Extracts -
 Comparison of Antibiotic Susceptibility Testing Results for Gram-Positive Mastitis Pathogens from Dairy Cows
Comparison of Antibiotic Susceptibility Testing Results for Gram-Positive Mastitis Pathogens from Dairy Cows -
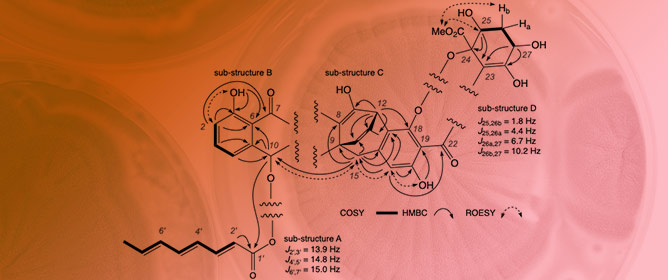 Jugiones A–D: Antibacterial Xanthone–Anthraquinone Heterodimers from Australian Soil-Derived Penicillium shearii CMB-STF067
Jugiones A–D: Antibacterial Xanthone–Anthraquinone Heterodimers from Australian Soil-Derived Penicillium shearii CMB-STF067
Journal Description
Antibiotics
Antibiotics
is an international, peer-reviewed, open access journal on all aspects of antibiotics, published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q1 (Pharmacology & Pharmacy) / CiteScore - Q1 (General Pharmacology, Toxicology and Pharmaceutics)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 13.7 days after submission; acceptance to publication is undertaken in 2.5 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
4.8 (2022);
5-Year Impact Factor:
4.9 (2022)
Latest Articles
Risk Factors and Outcomes of Patients Colonized with KPC and NDM Carbapenemase-Producing Enterobacterales
Antibiotics 2024, 13(5), 427; https://doi.org/10.3390/antibiotics13050427 - 8 May 2024
Abstract
Carbapenemase-producing enterobacterales (CPE) poses an increasing threat in hospitals worldwide. Recently, the prevalence of different carbapenemases conferring carbapenem resistance in enterobacterales changed in our country, including an increase in New Delhi Metallo-beta-lactamase (NDM)-CPE. We conducted a comparative historical study of adult patients colonized
[...] Read more.
Carbapenemase-producing enterobacterales (CPE) poses an increasing threat in hospitals worldwide. Recently, the prevalence of different carbapenemases conferring carbapenem resistance in enterobacterales changed in our country, including an increase in New Delhi Metallo-beta-lactamase (NDM)-CPE. We conducted a comparative historical study of adult patients colonized with Klebsiella pneumoniae carbapenemase (KPC)-CPE (July 2016 to June 2018, a historical cohort) vs. NDM-CPE (July 2016 to January 2023). We identified patients retrospectively through the microbiology laboratory and reviewed their files, extracting demographics, underlying diseases, Charlson Comorbidity Index (CCI) scores, treatments, and outcomes. This study included 228 consecutive patients from whom a CPE rectal swab screening was obtained: 136 NDM-CPE positive and 92 KPC-CPE positive. NDM-CPE-colonized patients had a shorter hospitalization length and a significantly lower 30-day post-discharge mortality rate (p = 0.002) than KPC-CPE-colonized patients. Based on multivariate regression, independent risk factors predicting CPE-NDM colonization included admission from home and CCI < 4 (p < 0.001, p = 0.037, respectively). The increase in NDM-CPE prevalence necessitates a modified CPE screening strategy upon hospital admission tailored to the changing local CPE epidemiology. In our region, the screening of younger patients residing at home with fewer comorbidities should be considered, regardless of a prior community healthcare contact or hospital admission.
Full article
(This article belongs to the Special Issue Epidemiology and Characterization of Bacteria Isolated from Hospital)
Open AccessArticle
Screening for Antibiotic Resistance Genes in Bacteria and the Presence of Heavy Metals in the Upstream and Downstream Areas of the Wadi Hanifah Valley in Riyadh, Saudi Arabia
by
Norah M. Al-Otaibi, Bassam Alsulaiman, Fahad M. Alreshoodi, Lenah E. Mukhtar, Sulaiman M. Alajel, Norah M. Binsaeedan and Fahad M. Alshabrmi
Antibiotics 2024, 13(5), 426; https://doi.org/10.3390/antibiotics13050426 - 8 May 2024
Abstract
Valley surface water is considered a focal public health concern owing to the presence of multi-drug-resistant bacteria. The distribution of antimicrobial resistance (AMR) bacteria in the surface water is affected by the presence of multiple factors, including antibiotics coming from wastewater discharge or
[...] Read more.
Valley surface water is considered a focal public health concern owing to the presence of multi-drug-resistant bacteria. The distribution of antimicrobial resistance (AMR) bacteria in the surface water is affected by the presence of multiple factors, including antibiotics coming from wastewater discharge or other contaminant sources such as pharmaceuticals, biocides, and heavy metals. Furthermore, there is evidence suggesting that high levels of antibiotic resistance genes (ARGs) can be transferred within bacterial communities under the influence of heavy metal stress. Hence, the primary aim of this study is to investigate the presence of heavy metals and bacterial ARGs in upstream as well as downstream locations of Wadi Hanifah Valley in Riyadh, Saudi Arabia. Sample collection was conducted at eighteen surface water sites within the valley in total. The selection of ARGs was associated with the most common antibiotics, including β-lactam, tetracycline, erythromycin, gentamicin, sulphonamide, chloramphenicol, vancomycin, trimethoprim, and colistin antibiotics, which were detected qualitatively using polymerase chain reaction (PCR) technology. The tested antibiotic resistance genes (ARGs) included (blaNDM-1 (for the antibiotic class Beta-lactamases), mecA (methicillin-resistant Staphylococcus aureus), tet(M) and tet(B) (for the antibiotic class Tetracycline), ampC (for the antibiotic class Beta-lactamases), vanA (for the antibiotic class vancomycin), mcr-1 (for the antibiotic class colistin), erm(B) (for the antibiotic class erythromycin), aac6′-Ie-aph2-Ia (for the antibiotic class Gentamicin), sulII (for the antibiotic class sulphonamide), catII (for the antibiotic class Chlorophincol), and dfrA1 (for the antibiotic class trimethoprim). Moreover, an assessment of the levels of heavy metals such as lithium (Li), beryllium (Be), chromium (Cr), cobalt (Co), arsenic (As), cadmium (Cd), tin (Sn), mercury (Hg), and lead (Pb) was conducted by using inductively coupled plasma mass spectrometry (ICPMS). According to our findings, the concentrations of sulphonamide, erythromycin, and chloramphenicol ARGs (erm(B), sulII, and catII) were observed to be the most elevated. Conversely, two ARGs, namely mecA and mcr-1, were not detected in the samples. Moreover, our data illustrated a significant rise in ARGs in the bacteria of water samples from the upstream sites as compared with the water samples from the downstream sites of Wadi Hanifah Valley. The mean concentration of Li, Be, Cr, Co, As, Cd, Sn, Hg, and Pb in the water samples was estimated to be 37.25 µg/L, 0.02 µg/L, 0.56 µg/L,0.32 µg/L, 0.93 µg/L, 0.01 µg/L, 200.4 µg/L, 0.027 µg/L, and 0.26 µg/L, respectively, for the selected 18 sites. Furthermore, it was revealed that the concentrations of the screened heavy metals in the water samples collected from various sites did not surpass the maximum limits set by the World Health Organization (WHO). In conclusion, this study offers a concise overview of the presence of heavy metals and ARGs in water samples obtained from the Wadi Hanifah Valley in Riyadh, KSA. Such findings will contribute to the ongoing monitoring and future risk assessment of ARGs spread in surface water.
Full article
(This article belongs to the Special Issue The Use of Antibiotics in Aquaculture: Antimicrobial Resistance, Efficacy and Safety, Ethical and Environmental Concerns)
►▼
Show Figures

Figure 1
Open AccessArticle
Validation of Serum Calprotectin Relative to Other Biomarkers of Infection in Febrile Infants Presenting to the Emergency Department
by
Mary Kathryn Bohn, Aleksandra Havelka, Mats Eriksson and Khosrow Adeli
Antibiotics 2024, 13(5), 425; https://doi.org/10.3390/antibiotics13050425 - 7 May 2024
Abstract
Antimicrobial stewardship involves a delicate balance between the risk of undertreating individuals and the potential societal burden of overprescribing antimicrobials. This balance is especially crucial in neonatal care. In this observational study, the usefulness of biomarkers of infectious diseases (calprotectin, procalcitonin (PCT), C-reactive
[...] Read more.
Antimicrobial stewardship involves a delicate balance between the risk of undertreating individuals and the potential societal burden of overprescribing antimicrobials. This balance is especially crucial in neonatal care. In this observational study, the usefulness of biomarkers of infectious diseases (calprotectin, procalcitonin (PCT), C-reactive protein (CRP), and white blood cells (WBCs) were evaluated in 141 febrile infants aged 28–90 days presenting to an emergency department. Since our focus was on the usefulness of serum calprotectin, this biomarker was not part of clinical decision-making. A significant difference was observed in the levels of all biomarkers, related to final discharge diagnosis and disposition status. The difference in levels related to antibiotic prescription was significant for all biomarkers but WBCs. The performance of calprotectin in the detection of bacterial infections (AUC (95% CI): 0.804 (0.691, 0.916)) was comparable to the performance of both PCT (0.901 (0.823, 0.980)) and CRP (0.859 (0.764, 0.953)) and superior to the WBC count (0.684 (0.544, 0.823)). Procalcitonin and CRP demonstrated a statistically significantly higher specificity relative to calprotectin. In this cohort, antibiotic use did not always correlate to a definite diagnosis of confirmed bacterial infection. The sample size was limited due to associated challenges with recruiting febrile infants. Hence, there is a need for adequate diagnostic tools to help discriminate between various kinds of infections. This study suggests serum calprotectin, procalcitonin, and CRP may serve as valuable biomarkers to differentiate between types of infection, in addition to clinical input and decision-making.
Full article
(This article belongs to the Special Issue Antibiotic Use and Antimicrobial Stewardship for Children in the Emergency Department)
►▼
Show Figures

Figure 1
Open AccessArticle
Efficacy of a Novel Prophylactic Scheme of Fosfomycin Trometamol in Patients Undergoing Endoscopic Surgery for Benign Prostatic Hyperplasia: Findings from a Prospective Monocentric Single-Arm Study
by
Pasquale Maria Berrino, Milo Gatti, Valeria Rotaru, Lorenzo Bianchi, Fabio Tumietto, Elena Sora, Riccardo Schiavina, Eugenio Brunocilla, Pierluigi Viale and Federico Pea
Antibiotics 2024, 13(5), 424; https://doi.org/10.3390/antibiotics13050424 - 6 May 2024
Abstract
This study aimed to assess the efficacy of a novel prophylactic scheme of fosfomycin trometamol in patients undergoing elective HoLEP (holmium laser enucleation of the prostate) or TURP (transurethral resection of the prostate) procedures for treating benign prostatic hyperplasia. Patients affected by benign
[...] Read more.
This study aimed to assess the efficacy of a novel prophylactic scheme of fosfomycin trometamol in patients undergoing elective HoLEP (holmium laser enucleation of the prostate) or TURP (transurethral resection of the prostate) procedures for treating benign prostatic hyperplasia. Patients affected by benign prostatic hyperplasia and undergoing elective HoLEP or TURP procedures during the period February 2022–June 2023 were prospectively enrolled. Two 3 g oral fosfomycin trometamol doses 12 h apart were administered at 8.00 p.m. on day −1 (i.e., the day before HoLEP or TURP procedure) and at 8.00 a.m. on day 0 (i.e., the day of the surgical procedure). The following outcomes were assessed: prevalence of fever occurring in the first 48 h after surgical procedure; prevalence of urological complications occurring after the surgical procedure; prevalence of proven urinary tract infections (UTIs) and/or bloodstream infections (BSIs) at 14 days post-procedure; and prevalence of emergency department admission for UTI-related sepsis at 14 days post-procedure. Univariate analysis comparing patients with and without proven UTI, BSI, or emergency department admission at 14 days post-procedure was carried out. Overall, 96 patients (median age 70 years) undergoing HoLEP (82.3%) or TURP (17.7%) were prospectively included. Median (IQR) time of surgical procedure after the morning fosfomycin dose was 226.5 min (range 88.5–393.75 min). Fever in the post-surgical 48 h occurred in 3/96 patients (3.1%). Prevalence of proven UTI at 14 days was as low as 1.0% (1/96), whereas no patient had proven BSI or UTI-related sepsis requiring emergency department admission at 14 days. Our findings support the contention that a prophylactic scheme based on two doses of fosfomycin trometamol 12 h apart before surgical intervention may represent a valuable strategy for preventing infectious complications in urologic patients undergoing HoLEP or TURP. Larger definitive confirmatory studies are warranted.
Full article
(This article belongs to the Special Issue Antimicrobial Prescribing and Antimicrobial Use in Healthcare Settings)
►▼
Show Figures
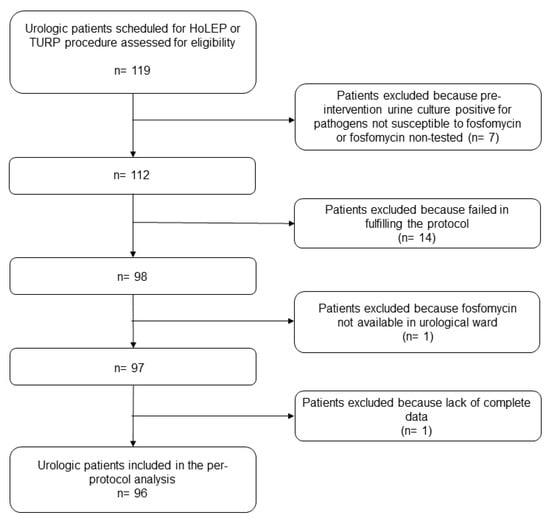
Figure 1
Open AccessReview
Treatment Strategies of Colistin Resistance Acinetobacter baumannii Infections
by
Andria Papazachariou, Renatos-Nikolaos Tziolos, Stamatis Karakonstantis, Petros Ioannou, George Samonis and Diamantis P. Kofteridis
Antibiotics 2024, 13(5), 423; https://doi.org/10.3390/antibiotics13050423 - 6 May 2024
Abstract
Acinetobacter baumannii has emerged as a pressing challenge in clinical practice, mainly due to the development of resistance to multiple antibiotics, including colistin, one of the last-resort treatments. This review highlights all the possible mechanisms of colistin resistance and the genetic basis contributing
[...] Read more.
Acinetobacter baumannii has emerged as a pressing challenge in clinical practice, mainly due to the development of resistance to multiple antibiotics, including colistin, one of the last-resort treatments. This review highlights all the possible mechanisms of colistin resistance and the genetic basis contributing to this resistance, such as modifications to lipopolysaccharide or lipid A structures, alterations in outer membrane permeability via porins and heteroresistance. In light of this escalating threat, the review also evaluates available treatment options. The development of new antibiotics (cefiderocol, sulbactam/durlobactam) although not available everywhere, and the use of various combinations and synergistic drug combinations (including two or more of the following: a polymyxin, ampicillin/sulbactam, carbapenems, fosfomycin, tigecycline/minocycline, a rifamycin, and aminoglycosides) are discussed in the context of overcoming colistin resistance of A. baumannii infections. Although most studied combinations are polymyxin-based combinations, non-polymyxin-based combinations have been emerging as promising options. However, clinical data remain limited and continued investigation is essential to determine optimal therapeutic strategies against colistin-resistant A. baumannii.
Full article
(This article belongs to the Special Issue Antibiotic Based Strategies for Prevention or Therapy of MDR Pneumonia)
Open AccessReview
Short-Chained Linear Scorpion Peptides: A Pool for Novel Antimicrobials
by
Tolis Panayi, Spiridoula Diavoli, Vicky Nicolaidou, Christos Papaneophytou, Christos Petrou and Yiannis Sarigiannis
Antibiotics 2024, 13(5), 422; https://doi.org/10.3390/antibiotics13050422 - 5 May 2024
Abstract
Scorpion venom peptides are generally classified into two main groups: the disulfide bridged peptides (DBPs), which usually target membrane-associated ion channels, and the non-disulfide bridged peptides (NDBPs), a smaller group with multifunctional properties. In the past decade, these peptides have gained interest because
[...] Read more.
Scorpion venom peptides are generally classified into two main groups: the disulfide bridged peptides (DBPs), which usually target membrane-associated ion channels, and the non-disulfide bridged peptides (NDBPs), a smaller group with multifunctional properties. In the past decade, these peptides have gained interest because most of them display functions that include antimicrobial, anticancer, haemolytic, and anti-inflammatory activities. Our current study focuses on the short (9–19 amino acids) antimicrobial linear scorpion peptides. Most of these peptides display a net positive charge of 1 or 2, an isoelectric point at pH 9–10, a broad range of hydrophobicity, and a Grand Average of Hydropathy (GRAVY) Value ranging between −0.05 and 1.7. These features allow these peptides to be attracted toward the negatively charged phospholipid head groups of the lipid membranes of target cells, a force driven by electrostatic interactions. This review outlines the antimicrobial potential of short-chained linear scorpion venom peptides. Additionally, short linear scorpion peptides are in general more attractive for large-scale synthesis from a manufacturing point of view. The structural and functional diversity of these peptides represents a good starting point for the development of new peptide-based therapeutics.
Full article
(This article belongs to the Special Issue Insights into Natural Antimicrobial Peptides)
►▼
Show Figures

Figure 1
Open AccessArticle
The MraY Inhibitor Muraymycin D2 and Its Derivatives Induce Enlarged Cells in Obligate Intracellular Chlamydia and Wolbachia and Break the Persistence Phenotype in Chlamydia
by
Iris Löckener, Lara Vanessa Behrmann, Jula Reuter, Andrea Schiefer, Anna Klöckner, Sebastian Krannich, Christian Otten, Katja Mölleken, Satoshi Ichikawa, Achim Hoerauf, Tanja Schneider, Kenneth M. Pfarr and Beate Henrichfreise
Antibiotics 2024, 13(5), 421; https://doi.org/10.3390/antibiotics13050421 - 4 May 2024
Abstract
Chlamydial infections and diseases caused by filarial nematodes are global health concerns. However, treatment presents challenges due to treatment failures potentially caused by persisting Chlamydia and long regimens against filarial infections accompanied by low compliance. A new treatment strategy could be the targeting
[...] Read more.
Chlamydial infections and diseases caused by filarial nematodes are global health concerns. However, treatment presents challenges due to treatment failures potentially caused by persisting Chlamydia and long regimens against filarial infections accompanied by low compliance. A new treatment strategy could be the targeting of the reduced peptidoglycan structures involved in cell division in the obligate intracellular bacteria Chlamydia and Wolbachia, the latter being obligate endosymbionts supporting filarial development, growth, and survival. Here, cell culture experiments with C. trachomatis and Wolbachia showed that the nucleoside antibiotics muraymycin and carbacaprazamycin interfere with bacterial cell division and induce enlarged, aberrant cells resembling the penicillin-induced persistence phenotype in Chlamydia. Enzymatic inhibition experiments with purified C. pneumoniae MraY revealed that muraymycin derivatives abolish the synthesis of the peptidoglycan precursor lipid I. Comparative in silico analyses of chlamydial and wolbachial MraY with the corresponding well-characterized enzyme in Aquifex aeolicus revealed a high degree of conservation, providing evidence for a similar mode of inhibition. Muraymycin D2 treatment eradicated persisting non-dividing C. trachomatis cells from an established penicillin-induced persistent infection. This finding indicates that nucleoside antibiotics may have additional properties that can break bacterial persistence.
Full article
(This article belongs to the Section Novel Antimicrobial Agents)
►▼
Show Figures
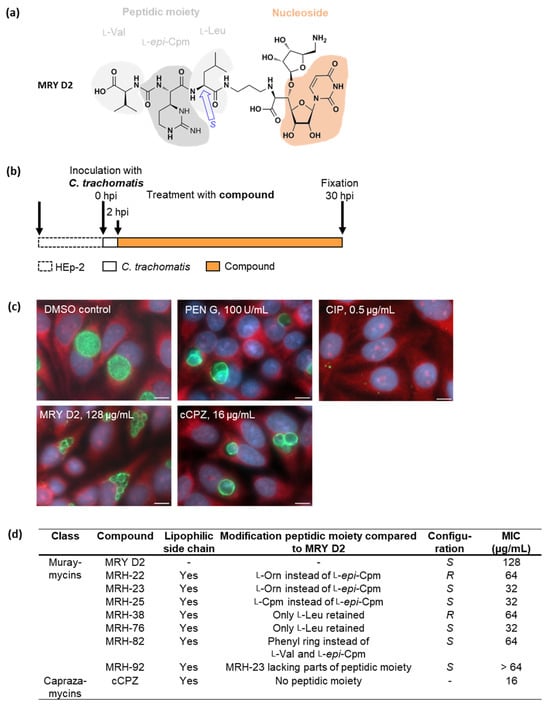
Figure 1
Open AccessArticle
A Qualitative Review of Patient Feedback for the OPAT (Outpatient Antimicrobial Therapy) Service in Bristol
by
Shuchita Soni, Irasha Harding, Carys Jones, Sue Wade, Jenna Norton and Jennifer Siobhan Pollock
Antibiotics 2024, 13(5), 420; https://doi.org/10.3390/antibiotics13050420 - 3 May 2024
Abstract
Outpatient parenteral antimicrobial therapy (OPAT) aims to deliver intravenous antimicrobials to medically stable patients with complex infections outside of a hospital setting. There is good evidence to demonstrate the safety and efficacy of OPAT in the literature. Anecdotally, the feedback from patients has
[...] Read more.
Outpatient parenteral antimicrobial therapy (OPAT) aims to deliver intravenous antimicrobials to medically stable patients with complex infections outside of a hospital setting. There is good evidence to demonstrate the safety and efficacy of OPAT in the literature. Anecdotally, the feedback from patients has been positive, but only a few studies evaluate this topic in detail. The aim of this qualitative study was to examine patients’ experiences with and feedback on the OPAT service in Bristol, United Kingdom, which was established in 2021. A total of 92 patient feedback surveys were reviewed retrospectively, and thematic analysis was undertaken. Feedback from OPAT patients in our centre was overwhelmingly positive. The key themes identified were benefits to the patients, their friends, and family, and positive feedback about OPAT staff. The mean overall satisfaction score for OPAT was 9.6 out of 10. Areas to improve included communication between the OPAT and parent teams, improving OPAT capacity, and expansion of the service.
Full article
(This article belongs to the Section Antibiotic Therapy in Infectious Diseases)
Open AccessFeature PaperArticle
Meropenem Disposition in Neonatal and Pediatric Extracorporeal Membrane Oxygenation and Continuous Renal Replacement Therapy
by
Pavla Pokorná, Danica Michaličková, Dick Tibboel and Jonas Berner
Antibiotics 2024, 13(5), 419; https://doi.org/10.3390/antibiotics13050419 - 3 May 2024
Abstract
This study aimed to characterize the impact of extracorporeal membrane oxygenation (ECMO) on the pharmacokinetics (PK) of meropenem in neonates and children and to provide recommendations for meropenem dosing in this specific population of patients. Therapeutic drug monitoring (152 meropenem plasma concentrations) data
[...] Read more.
This study aimed to characterize the impact of extracorporeal membrane oxygenation (ECMO) on the pharmacokinetics (PK) of meropenem in neonates and children and to provide recommendations for meropenem dosing in this specific population of patients. Therapeutic drug monitoring (152 meropenem plasma concentrations) data from 45 patients (38 received ECMO) with a body weight (BW) of 7.88 (3.62–11.97) kg (median (interquartile range)) and postnatal age of 3 (0–465) days were collected. The population PK analysis was performed using NONMEM V7.3.0. Monte Carlo simulations were performed to assess the probability of target achievement (PTA) for 40% of time the free drug remained above the minimum inhibitory concentration (fT > MIC) and 100% fT > MIC. BW was found to be a significant covariate for the volume of distribution (Vd) and clearance (CL). Additionally, continuous renal replacement therapy (CRRT) was associated with a two-fold increase in Vd. In the final model, the CL and Vd for a typical patient with a median BW of 7.88 kg that was off CRRT were 1.09 L/h (RSE = 8%) and 3.98 L (14%), respectively. ECMO did not affect meropenem PK, while superimposed CRRT significantly increased Vd. We concluded that current dosing regimens provide acceptably high PTA for MIC ≤ 4 mg/L for 40% fT > MIC, but individual dose adjustments are needed for 100% fT > MIC.
Full article
(This article belongs to the Special Issue Pharmacokinetic and Antibiotic Dosing for Intensive Care Unit Patients)
►▼
Show Figures

Figure 1
Open AccessArticle
Flow Cytometry as a Rapid and Valuable Method in Investigation of Colistin Resistance in Carbapenem-Resistant Klebsiella pneumoniae Isolates
by
Şafak Ceren Uçak and Betigül Öngen
Antibiotics 2024, 13(5), 418; https://doi.org/10.3390/antibiotics13050418 - 2 May 2024
Abstract
Rapid detection of antimicrobial resistance is crucial for early initiation of appropriate therapy. The aim of this study was to investigate whether resistance to colistin, the last-resort antibiotic, in carbapenem-resistant Klebsiella pneumoniae (CRKP) isolates can be detected accurately and rapidly by flow cytometry
[...] Read more.
Rapid detection of antimicrobial resistance is crucial for early initiation of appropriate therapy. The aim of this study was to investigate whether resistance to colistin, the last-resort antibiotic, in carbapenem-resistant Klebsiella pneumoniae (CRKP) isolates can be detected accurately and rapidly by flow cytometry (FCM). The VITEK 2 automated system was used to identify 85 K. pneumoniae strains and to determine their resistance to carbapenems. The minimum inhibitory concentration (MIC) values for colistin in 85 CRKP strains were determined by broth microdilution (BMD), which is the reference method. In addition, FCM was used, combined with DiBAC4(3) fluorescent stain, to determine colistin susceptibility. The MIC₅₀ value of the strains, 80% of which were resistant to colistin by the BMD method, was 16 mg/L, and the MIC₉₀ value was 32 mg/L. When FCM was compared with the reference method, it was determined that the specificity was 94.1%, sensitivity was 100% of FCM, and Cohen’s kappa value was 0.96. Colistin susceptibility results with FCM were obtained within an average of 2 h. These findings suggest that FCM holds great promise as a rapid and reliable alternative method for detecting colistin resistance in CRKP strains.
Full article
(This article belongs to the Section Antibiotic Therapy in Infectious Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
Occurrence of Antimicrobial-Resistant Enterococcus spp. in Healthy Chickens Never Exposed to Antimicrobial Agents in Central Italy
by
Giulia Cagnoli, Alessia Di Paolo, Fabrizio Bertelloni, Sonia Salvucci, Arianna Buccioni, Margherita Marzoni Fecia di Cossato and Valentina Virginia Ebani
Antibiotics 2024, 13(5), 417; https://doi.org/10.3390/antibiotics13050417 - 1 May 2024
Abstract
Enterococci are part of the natural flora of the gastrointestinal tract of mammals, including humans, birds and invertebrates. They can cause infection, mainly among hospitalized patients, as well as acquire and transfer antimicrobial resistance genes. The present study allowed the isolation of 98
[...] Read more.
Enterococci are part of the natural flora of the gastrointestinal tract of mammals, including humans, birds and invertebrates. They can cause infection, mainly among hospitalized patients, as well as acquire and transfer antimicrobial resistance genes. The present study allowed the isolation of 98 Enterococcus (73.47% E. faecium, 23.47% E. faecalis, 3.06% E. avium) strains from 120-day-old healthy chickens that had never been treated with antimicrobials. Their antimicrobial resistance was evaluated by the agar disk diffusion method; high-level aminoglycoside (streptomycin and gentamicin) and vancomycin resistance were established using the microbroth dilution method. The highest percentages of resistant isolates were detected with quinupristin–dalfopristin (88.78%), rifampicin (64.29%), tetracyclines (45.92%), and enrofloxacin (41.84%). High percentages of susceptible strains were found with teicoplanin (100%), amoxicillin–clavulanic acid (97.96%), nitrofurantoin (94.90%), ampicillin (92.86%), chloramphenicol (90.82%), and linezolid (88.78%). About 60% of the strains were classified as MDR (multidrug-resistant). Moreover, PCR was carried out to investigate genes encoding for tetracyclines resistance determinants: tet(M), tet(L), tet(O), tet(K), and Int-Tn. Genes were detected in 68 (69.38%) strains: 36 were shown to be resistant with the agar disk diffusion method, while 28 were intermediate, and 2 were susceptible. The present study showed that chickens never treated with antimicrobials potentially harbor enterococci having phenotypic and genotypic characters of antimicrobial resistance.
Full article
(This article belongs to the Special Issue Detection of Bacteria and Antibiotics Surveillance in Livestock)
Open AccessBrief Report
Comparative In Vitro Activity of Ceftazidime-Avibactam, Imipenem-Relebactam, and Meropenem-Vaborbactam against Carbapenem-Resistant Clinical Isolates of Klebsiella pneumoniae and Pseudomonas aeruginosa
by
Anthony Sophonsri, Michelle Kalu and Annie Wong-Beringer
Antibiotics 2024, 13(5), 416; https://doi.org/10.3390/antibiotics13050416 - 1 May 2024
Abstract
Co-infection with carbapenem-resistant Klebsiella pneumoniae (CRKP) and Pseudomonas aeruginosa (CRPA) is associated with poor outcomes and historically relied on combination therapy with toxic agents for management. However, several novel β-lactam/β-lactamase inhibitor combination agents have been developed, offering potential monotherapy options. Here, we compare
[...] Read more.
Co-infection with carbapenem-resistant Klebsiella pneumoniae (CRKP) and Pseudomonas aeruginosa (CRPA) is associated with poor outcomes and historically relied on combination therapy with toxic agents for management. However, several novel β-lactam/β-lactamase inhibitor combination agents have been developed, offering potential monotherapy options. Here, we compare the in vitro activity of ceftazidime-avibactam (CZA), imipenem-relebactam (IRL), and meropenem-vaborbactam (MVB) against both CRKP and CRPA clinical isolates. Minimum inhibitory concentrations (MICs) for each agent were determined using broth microdilution. Carbapenemase gene detection was performed for representative isolates of varying carbapenem resistance phenotypes. IRL demonstrated excellent activity against CRKP and CRPA with susceptibility rates at 95.8% and 91.7%, respectively. While CZA and MVB showed comparable susceptibility to IRL against CRKP (93.8%), susceptibility of CRPA to CZA was modest at 79.2%, whereas most CRPA strains were resistant to MVB. Of the 35 CRKP isolates tested, 91.4% (32/35) carried a blaKPC gene. Only 1 of 37 (2.7%) CRPA isolates tested carried a blaVIM gene, which conferred phenotypic resistance to all three agents. None of the CRKP strains were cross-resistant to all three agents. Source of infection and co-infection did not significantly influence antimicrobial activity for IRL and CZA; none of the CRPA isolates from co-infected patients were susceptible to MVB. Our results suggest that novel β-lactam agents with antipseudomonal activity and stability against carbapenemases, such as IRL and CZA, offer potential monotherapy options for the treatment of co-infection involving both CRKP and CRPA, but not MVB.
Full article
(This article belongs to the Special Issue Carbapenemases in Gram-Negative Bacteria: A Global Health Threat and Therapeutic Challenge)
►▼
Show Figures
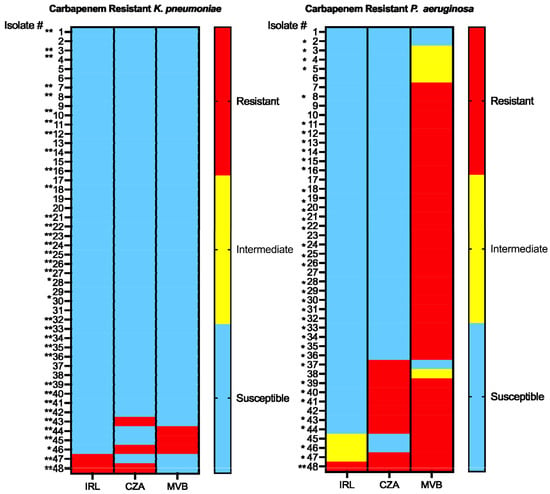
Figure 1
Open AccessReview
Natural Antimicrobials in Dairy Products: Benefits, Challenges, and Future Trends
by
Maria Eduarda Marques Soutelino, Adriana Cristina de Oliveira Silva and Ramon da Silva Rocha
Antibiotics 2024, 13(5), 415; https://doi.org/10.3390/antibiotics13050415 - 1 May 2024
Abstract
This review delves into using natural antimicrobials in the dairy industry and examines various sources of these compounds, including microbial, plant, and animal sources. It discusses the mechanisms by which they inhibit microbial growth, for example, by binding to the cell wall’s precursor
[...] Read more.
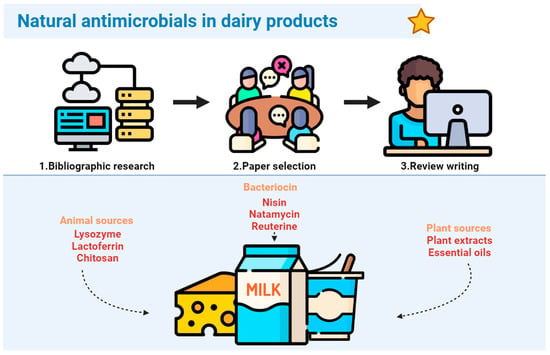
This review delves into using natural antimicrobials in the dairy industry and examines various sources of these compounds, including microbial, plant, and animal sources. It discusses the mechanisms by which they inhibit microbial growth, for example, by binding to the cell wall’s precursor molecule of the target microorganism, consequently inhibiting its biosynthesis, and interfering in the molecule transport mechanism, leading to cell death. In general, they prove to be effective against the main pathogens and spoilage found in food, such as Escherichia coli, Staphylococcus aureus, Bacillus spp., Salmonella spp., mold, and yeast. Moreover, this review explores encapsulation technology as a promising approach for increasing the viability of natural antimicrobials against unfavorable conditions such as pH, temperature, and oxygen exposure. Finally, this review examines the benefits and challenges of using natural antimicrobials in dairy products. While natural antimicrobials offer several advantages, including improved safety, quality, and sensory properties of dairy products, it is crucial to be aware of the challenges associated with their use, such as potential allergenicity, regulatory requirements, and consumer perception. This review concludes by emphasizing the need for further research to identify and develop effective and safe natural antimicrobials for the dairy industry to ensure the quality and safety of dairy products for consumers.
Full article
(This article belongs to the Special Issue Updates on Major Food-Related Pathogens: Antimicrobial Treatment, Drug Resistance, Inactivation, and Related Diseases)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Bacitracin Methylene Disalicylate (BMD) Treatment Affects Spleen Proteome in Broiler Chicks Infected with Salmonella enteritidis
by
Adedeji Adetunji, Theresa Casey, Uma K. Aryal, Tunde Ogundare, Jackeline Franco and Yewande Fasina
Antibiotics 2024, 13(5), 414; https://doi.org/10.3390/antibiotics13050414 - 1 May 2024
Abstract
Bacitracin Methylene Disalicylate (BMD), as a feed additive to poultry diets, enhances digestion, prevents Salmonella enteritidis (SE) colonization, and treats current infections. The objective of this study was to utilize a quantitative proteomic approach to determine the effect of BMD feed additive on
[...] Read more.
Bacitracin Methylene Disalicylate (BMD), as a feed additive to poultry diets, enhances digestion, prevents Salmonella enteritidis (SE) colonization, and treats current infections. The objective of this study was to utilize a quantitative proteomic approach to determine the effect of BMD feed additive on broiler chickens challenged with SE in the spleen proteome. At 1 d of age, chicks were randomly allocated into four groups: control with and without SE challenge (CON, n = 60; CON-SE, n = 60), BMD with and without SE challenge (BMD, n = 60; BMD-SE, n = 60). Birds in the CON-SE and BMD-SE treatment were administered SE inoculum by oral gavage. On day three and day seven post-gavage, the spleen was collected aseptically from birds in each treatment group (CON, n = 4/day; CON-SE, n = 4/day; BMD, n = 4/day; BMD-SE, n = 4/day). Proteomic analysis by liquid chromatography-tandem mass spectrometry (LC-MS/MS) showed an increased abundance of 115 proteins and decreased of 77 due to the BMD. Proteins that decreased in abundance were enriched for fibrinogen complex and extracellular space, whereas proteins that increased in abundance were enriched for proteasome-mediated ubiquitin-dependent protein catabolic process and mitochondrion. Analysis of the interaction between BMD and the Salmonella challenge found 230 differentially abundant proteins including proteins associated with RNA binding, spliceosome, protein transport, and cell adhesion among the upregulated proteins, and those associated with protein folding, carbon metabolism, biosynthesis of nucleotide sugars, response to oxidative stress, positive regulation of NIK/NF-kappaB signaling, and inflammatory response among the downregulated proteins. The impact of BMD treatment on spleen proteome indicates an anti-apoptotic effect. BMD also modified the response of the spleen to the SE challenge with a marked decrease in proteins that prompt cytokine synthesis and an increase in proteins involved in the selective removal of unfolded proteins.
Full article
(This article belongs to the Topic Animal Diseases in Agricultural Production Systems, 2nd Edition)
►▼
Show Figures
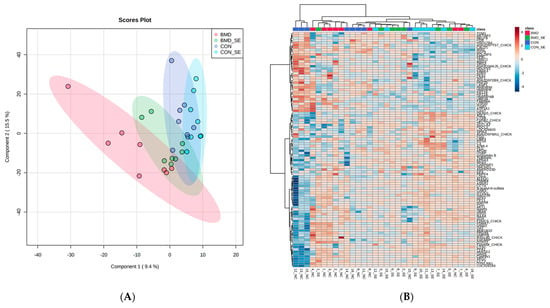
Figure 1
Open AccessArticle
Antibiotic Cocktail Effects on Intestinal Microbial Community, Barrier Function, and Immune Function in Early Broiler Chickens
by
Waseem Abbas, Ruichen Bi, Muhammad Dilshad Hussain, Alia Tajdar, Fangshen Guo, Yuming Guo and Zhong Wang
Antibiotics 2024, 13(5), 413; https://doi.org/10.3390/antibiotics13050413 - 30 Apr 2024
Abstract
This study investigated the effects of an antibiotic cocktail on intestinal microbial composition, mechanical barrier structure, and immune functions in early broilers. One-day-old healthy male broiler chicks were treated with a broad-spectrum antibiotic cocktail (ABX; neomycin, ampicillin, metronidazole, vancomycin, and kanamycin, 0.5 g/L
[...] Read more.
This study investigated the effects of an antibiotic cocktail on intestinal microbial composition, mechanical barrier structure, and immune functions in early broilers. One-day-old healthy male broiler chicks were treated with a broad-spectrum antibiotic cocktail (ABX; neomycin, ampicillin, metronidazole, vancomycin, and kanamycin, 0.5 g/L each) or not in drinking water for 7 and 14 days, respectively. Sequencing of 16S rRNA revealed that ABX treatment significantly reduced relative Firmicutes, unclassified Lachnospiraceae, unclassified Oscillospiraceae, Ruminococcus torques, and unclassified Ruminococcaceae abundance in the cecum and relative Firmicutes, Lactobacillus and Baccillus abundance in the ileum, but significantly increased richness (Chao and ACE indices) and relative Enterococcus abundance in the ileum and cecum along with relatively enriched Bacteroidetes, Proteobacteria, Cyanobacteria, and Enterococcus levels in the ileum following ABX treatment for 14 days. ABX treatment for 14 days also significantly decreased intestinal weight and length, along with villus height (VH) and crypt depth (CD) of the small intestine, and remarkably increased serum LPS, TNF-α, IFN-γ, and IgG levels, as well as intestinal mucosa DAO and MPO activity. Moreover, prolonged use of ABX significantly downregulated occludin, ZO-1, and mucin 2 gene expression, along with goblet cell numbers in the ileum. Additionally, chickens given ABX for 14 days had lower acetic acid, butyric acid, and isobutyric acid content in the cecum than the chickens treated with ABX for 7 days and untreated chickens. Spearman correlation analysis found that those decreased potential beneficial bacteria were positively correlated with gut health-related indices, while those increased potential pathogenic strains were positively correlated with gut inflammation and gut injury-related parameters. Taken together, prolonged ABX application increased antibiotic-resistant species abundance, induced gut microbiota dysbiosis, delayed intestinal morphological development, disrupted intestinal barrier function, and perturbed immune response in early chickens. This study provides a reliable lower-bacteria chicken model for further investigation of the function of certain beneficial bacteria in the gut by fecal microbiota transplantation into germ-free or antibiotic-treated chickens.
Full article
(This article belongs to the Special Issue Use of Antibiotics in Animals and Antimicrobial Resistance)
Open AccessCorrection
Correction: Lungu et al. Molecular Characterisation of Antimicrobial Resistance in E. coli Isolates from Piglets in the West Region of Romania. Antibiotics 2023, 12, 1544
by
Bianca Cornelia Lungu, Ioan Hutu and Paul Andrew Barrow
Antibiotics 2024, 13(5), 412; https://doi.org/10.3390/antibiotics13050412 - 30 Apr 2024
Abstract
The authors Bianca Cornelia Lungu and Ioan Hutu did not state contributed equally [...]
Full article
Open AccessReview
The Ongoing Debate on the Use of Prophylactic Antibiotics in Acute Pancreatitis—Is There a Conclusion? A Comprehensive Narrative Review
by
Kai Siang Chan and Vishal G. Shelat
Antibiotics 2024, 13(5), 411; https://doi.org/10.3390/antibiotics13050411 - 30 Apr 2024
Abstract
Acute pancreatitis (AP) is a common but often self-limiting disease in the majority of patients. However, in the minority, who may progress to moderately severe or severe AP, high mortality risk has been reported. Infected pancreatitis necrosis (IPN) in necrotising pancreatitis has been
[...] Read more.
Acute pancreatitis (AP) is a common but often self-limiting disease in the majority of patients. However, in the minority, who may progress to moderately severe or severe AP, high mortality risk has been reported. Infected pancreatitis necrosis (IPN) in necrotising pancreatitis has been shown to result in more than twice the mortality rate compared with in sterile pancreatic necrosis. This raises the question on whether prophylactic antibiotics (PABs) should be given in subgroups of AP to prevent superimposed infection to improve survival outcomes. Despite numerous randomised controlled trials (RCTs), meta-analyses, and guidelines on the management of AP, there is a lack of strong evidence to suggest the use of PABs in AP. Additionally, use of PABs is associated with antimicrobial resistance. Considerable heterogeneity exists and limits the interpretation of results—subgroup of AP benefitting from PAB use, choice/class of PAB, and timing of administration from symptom onset and duration of PAB use. Only a minority of existing meta-analyses suggest mortality benefits and reduction in IPN. The majority of existing guidelines do not recommend the use of PABs in AP. More research is required to make more definitive conclusions. Currently, PAB should only be administered after multidisciplinary discussions led by pancreatology experts.
Full article
(This article belongs to the Special Issue Antibiotic Use and the Emergence of Antibiotic Resistance in Clinical Settings)
►▼
Show Figures
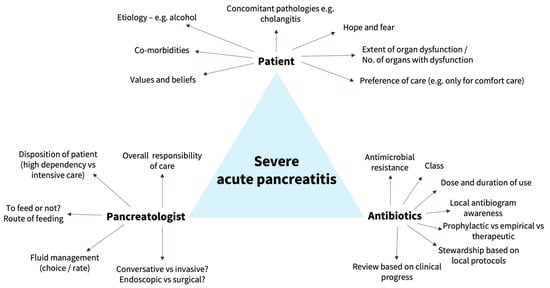
Figure 1
Open AccessReview
Linking S. aureus Immune Evasion Mechanisms to Staphylococcal Vaccine Failures
by
Irshad Ahmed Hajam and George Y. Liu
Antibiotics 2024, 13(5), 410; https://doi.org/10.3390/antibiotics13050410 - 30 Apr 2024
Abstract
Vaccination arguably remains the only long-term strategy to limit the spread of S. aureus infections and its related antibiotic resistance. To date, however, all staphylococcal vaccines tested in clinical trials have failed. In this review, we propose that the failure of S. aureus
[...] Read more.
Vaccination arguably remains the only long-term strategy to limit the spread of S. aureus infections and its related antibiotic resistance. To date, however, all staphylococcal vaccines tested in clinical trials have failed. In this review, we propose that the failure of S. aureus vaccines is intricately linked to prior host exposure to S. aureus and the pathogen’s capacity to evade adaptive immune defenses. We suggest that non-protective immune imprints created by previous exposure to S. aureus are preferentially recalled by SA vaccines, and IL-10 induced by S. aureus plays a unique role in shaping these non-protective anti-staphylococcal immune responses. We discuss how S. aureus modifies the host immune landscape, which thereby necessitates alternative approaches to develop successful staphylococcal vaccines.
Full article
(This article belongs to the Special Issue Staphylococcal Biology and Pathogenesis)
►▼
Show Figures
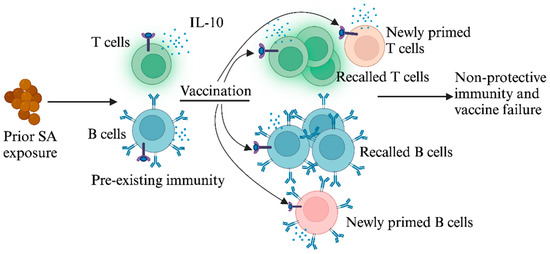
Figure 1
Open AccessArticle
The Genetic Landscape of Antimicrobial Resistance Genes in Enterococcus cecorum Broiler Isolates
by
Yue Huang, Filip Boyen, Gunther Antonissen, Nick Vereecke and Filip Van Immerseel
Antibiotics 2024, 13(5), 409; https://doi.org/10.3390/antibiotics13050409 - 29 Apr 2024
Abstract
Enterococcus cecorum is associated with bacterial chondronecrosis with osteomyelitis (BCO) in broilers. Prophylactic treatment with antimicrobials is common in the poultry industry, and, in the case of outbreaks, antimicrobial treatment is needed. In this study, the minimum inhibitory concentrations (MICs) and epidemiological cutoff
[...] Read more.
Enterococcus cecorum is associated with bacterial chondronecrosis with osteomyelitis (BCO) in broilers. Prophylactic treatment with antimicrobials is common in the poultry industry, and, in the case of outbreaks, antimicrobial treatment is needed. In this study, the minimum inhibitory concentrations (MICs) and epidemiological cutoff (ECOFF) values (COWT) for ten antimicrobials were determined in a collection of E. cecorum strains. Whole-genome sequencing data were analyzed for a selection of these E. cecorum strains to identify resistance determinants involved in the observed phenotypes. Wild-type and non-wild-type isolates were observed for the investigated antimicrobial agents. Several antimicrobial resistance genes (ARGs) were detected in the isolates, linking phenotypes with genotypes for the resistance to vancomycin, tetracycline, lincomycin, spectinomycin, and tylosin. These detected resistance genes were located on mobile genetic elements (MGEs). Point mutations were found in isolates with a non-wild-type phenotype for enrofloxacin and ampicillin/ceftiofur. Isolates showing non-wild-type phenotypes for enrofloxacin had point mutations within the GyrA, GyrB, and ParC proteins, while five amino acid changes in penicillin-binding proteins (PBP2x superfamily) were observed in non-wild-type phenotypes for the tested β-lactam antimicrobials. This study is one of the first that describes the genetic landscape of ARGs within MGEs in E. cecorum, in association with phenotypical resistance determination.
Full article
(This article belongs to the Special Issue Antibiotics Resistance in Animals and the Environment)
►▼
Show Figures

Figure 1
Open AccessArticle
Adsorption of Macrolide Antibiotics and a Metabolite onto Polyethylene Terephthalate and Polyethylene Microplastics in Aquatic Environments
by
Carmen Mejías, Julia Martín, Laura Martín-Pozo, Juan Luis Santos, Irene Aparicio and Esteban Alonso
Antibiotics 2024, 13(5), 408; https://doi.org/10.3390/antibiotics13050408 - 29 Apr 2024
Abstract
Microplastics (MPs) and antibiotics are emerging pollutants widely found in aquatic environments, potentially causing environmental harm. MPs may act as carriers for antibiotics, affecting their environmental distribution. This study investigates the adsorption of four macrolide antibiotics and a metabolite onto two types of
[...] Read more.
Microplastics (MPs) and antibiotics are emerging pollutants widely found in aquatic environments, potentially causing environmental harm. MPs may act as carriers for antibiotics, affecting their environmental distribution. This study investigates the adsorption of four macrolide antibiotics and a metabolite onto two types of MPs: polyethylene terephthalate (PET) and polyethylene (PE). Results revealed a linear isotherm adsorption model, with higher adsorption to PET than to PE (R2 > 0.936 for PE and R2 > 0.910 for PET). Hydrophobic interactions and hydrogen bonding could be the main adsorption mechanisms, with pore filling potentially involved. Reduced particle size enhances adsorption due to the increase of active adsorption sites. This increasement is more pronounced in PE than in PET, leading to an 11.6% increase in the average adsorption of all macrolides to PE, compared to only 5.1% to PET. Dissolved organic matter inhibits adsorption (azithromycin adsorption to PE was reduced from 12% to 5.1%), while salinity enhances it just until 1% salinity. pH slightly influences adsorption, with maximal adsorption at neutral pH. Results in real samples showed that complexity of the matrix decreased adsorption. Overall, these findings indicate that PE and PET MPs can be a vector of macrolides in aquatic environments.
Full article
(This article belongs to the Special Issue Environmental Fate and Effects of Antibiotics and Antibiotic Resistance Genes)
►▼
Show Figures

Figure 1

Journal Menu
► ▼ Journal Menu-
- Antibiotics Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Antibiotics, Antioxidants, JoF, Microbiology Research, Microorganisms
Redox in Microorganisms, 2nd Edition
Topic Editors: Michal Letek, Volker BehrendsDeadline: 31 July 2024
Topic in
Antibiotics, JPM, Pharmaceuticals, Pharmaceutics
Pharmacokinetic and Pharmacodynamic Modelling in Drug Discovery and Development
Topic Editors: Inaki F. Troconiz, Victor Mangas Sanjuán, Maria Garcia-Cremades MiraDeadline: 31 August 2024
Topic in
Molecules, Pharmaceutics, Antibiotics, Microorganisms, Biomolecules, Marine Drugs, Polymers, IJMS
Antimicrobial Agents and Nanomaterials
Topic Editors: Sandra Pinto, Vasco D. B. BonifácioDeadline: 30 September 2024
Topic in
Antibiotics, Biomedicines, JCM, Pharmaceuticals, Pharmaceutics
Challenges and Future Prospects of Antibacterial Therapy
Topic Editors: Kwang-sun Kim, Zehra EdisDeadline: 31 October 2024

Conferences
Special Issues
Special Issue in
Antibiotics
Development and Biomedical Application of Antibacterial Coatings
Guest Editor: Selvaraj Rajesh KumarDeadline: 10 May 2024
Special Issue in
Antibiotics
Antibacterial Treatment in Periodontal and Endodontic Therapy, 2nd Volume
Guest Editors: Andreas Braun, Felix KrauseDeadline: 15 May 2024
Special Issue in
Antibiotics
The Application of Antibiotic Therapy in Oral Surgery and Dental Implant Procedures
Guest Editors: Eugenio Velasco-Ortega, Angel-Orion Salgado-Peralvo, Juan Francisco Peña-CardellesDeadline: 31 May 2024
Special Issue in
Antibiotics
Challenges for Therapeutic Drug Monitoring of Antimicrobials
Guest Editors: Giuseppe Pipitone, Giuseppe Nunnari, Fabrizio TagliettiDeadline: 15 June 2024
Topical Collections
Topical Collection in
Antibiotics
Antimicrobial Resistance and Anti-Biofilms
Collection Editors: Ding-Qiang Chen, Yulong Tan, Ren-You Gan, Guanggang Qu, Zhenbo Xu, Junyan Liu








